I recently had the pleasure of speaking with Patty Taylor, Vice President, Professional Education and Clinical Affairs at Ansell, about the current state of infection control. We started our conversation off on a high note: the CDC released their HAI progress report in January, and the news is good. In reference to these victories, and throughout the interview Taylor kept returning to two themes: the front-line presence of Infection Control (IC) personnel, and the importance of continuous improvement.
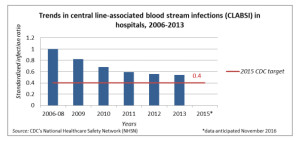
HAIs only show up in the news when there is a crisis. Within the last year, the two biggest stories have been the struggle with Ebola, and the recent superbug incidents on the West Coast. With more than 30 years working in infection control, Taylor has seen these sorts of crises come and go, and insists on the importance of building and maintaining infection control standards. Her perspective is borne out by the progress shown in the CDC report:
These graphs don’t show the peaks and valleys of media interest in HAIs, but rather the slow and steady improvement that Taylor is confident will continue.
Standards
If there was anything that Taylor credited with the reduction in HAIs, it was the maintenance of infection control standards, and the professionals to carry them out. “Certainly, infection control nurses have been at the forefront of increasing best practices throughout a hospital,” Taylor said. “They have a very important role in a hospital, and they’re looked to by hospital workers for guidance and counseling to handle certain situations.”
“I think a combination of education, monitoring, observation, and auditing, and repeating those are very important. And reinforce it — reinforcement of good behavior, too, is very important.”
Taylor offered the recent Ebola episode as an example of all these pieces working together. The different stakeholders involved “talked about the risk, about what was happening, about best practices, and they made changes right away to the training and the practice. They made sure that people were confident, and then they added routine observation.”
Technology
Taylor’s company, Ansell, takes a holistic approach to infection control. Ansell is part of the IC training infrastructure, providing an arsenal of resources for IC professionals, from something as straightforward as standardized hand-cleaning protocols to in-depth continuing education courses. But that total approach isn’t complete without technology that can fill in gaps. As Taylor makes clear, glove misuse is one of the most common mistakes in IC everyday practice.
“I think education and awareness will help increase the appropriate use of medical gloves, just like it has helped with hand hygiene, there’s no doubt in my mind. But the other challenge we have is behavior modification,” Taylor said. “Sometimes some new innovative products will help compensate for that individual who doesn’t change their behavior based on the education and knowledge they’ve been provided.”
Workload
When I asked Taylor if she could change one thing about the field, she said she would “provide more infection control nurses in the hospitals.”
“There’s certainly a shortage of nurses globally. I can’t speak for any one hospital, but globally there is a shortage of nurses.” IC personnel today are certainly dealing with a heavy workload. While the outpatient revolution has been great for patients, it also means that those patients still in the hospital are sicker than ever. Even the best trained personnel, with well-established standards, the latest in technology, and a great team can only do so much.
“We know what needs to be done. But nurses are faced with a heavy workload, sicker patients, a more multi-drug bacteria in the hospitals, so there’s a challenge there.”
Taylor concluded with a reminder of the stakes, “Patients should feel that, when they go into a hospital, they’re healthy that they won’t acquire an infection while they’re in the care of a hospital. We just want to make it better, we want to make sure patients are safe, and provide them a safe environment.”
While there have been great strides, making further progress in HAI reduction will mean increasing energy behind sustaining and improving best practices. “We just need to keep doing what we’re doing: education, awareness, setting policies and procedures, following up, being a good steward, talking to our colleagues. When we see that they’re not following best practice, to remind them of best practice.”
Source: www.surgicalproductsmag.com